More than a year into the pandemic, deaths in Brazil are now at their peak. But despite the overwhelming evidence that Covid-19 rarely kills young children, in Brazil 1,300 babies have died from the virus. One doctor refused to test Jessika Ricarte’s one-year-old son for Covid, saying his symptoms did not fit the profile of the virus. Two months later he died of complications from the disease.
After two years of trying, and failed fertility treatments, teacher Jessika Ricarte had all but given up on having a family. Then she fell pregnant with Lucas.
“His name comes from luminous. And he was a light in our life. He showed that happiness was much more than we imagined,” she says.

She first suspected something was wrong when Lucas, always a good eater, lost his appetite.
At first Jessika wondered if he was teething. Lucas’s godmother, a nurse, suggested that he might just have a sore throat. But after he developed a fever, then fatigue and slightly laboured breathing, Jessika took him to hospital, and asked for him to be tested for Covid.
“The doctor put on the oximeter. Lucas’s levels were 86%. Now I know that is not normal,” says Jessika.
But he was not feverish, so the doctor said: “My dear, don’t worry. There’s no need for a Covid test. It’s probably just a minor sore throat.”
He told Jessika that Covid-19 was rare in children, gave her some antibiotics and sent her home. Despite her misgivings, there was no option to have Lucas tested privately at the time.
Jessika says that some of his symptoms dissipated at the end of his 10-day antibiotics course, but the tiredness remained – as did her concerns about coronavirus.
“I sent several videos to his godmother, my parents, my mother-in-law, and everyone said that I was exaggerating, that I should stop watching the news, that it was making me paranoid. But I knew that my son was not himself, that he was not breathing normally.”

This was May 2020, and the coronavirus epidemic was growing. Two people had already died in her town, Tamboril in Ceará, north-east Brazil. “Everyone knows each other here. The town was in shock.”
Jessika’s husband Israel was worried that another hospital visit would increase the risk that she and Lucas would become infected with the virus.
But the weeks went by, and Lucas became sleepier and sleepier. Finally on 3 June, Lucas vomited over and over again after eating lunch, and Jessika knew she had to act.
They returned to their local hospital, where the doctor tested Lucas for Covid, to rule it out.
Lucas’s godmother, who worked there, broke the news to the couple that his test result was positive.
“At the time, the hospital did not even have a resuscitator,” says Jessika.
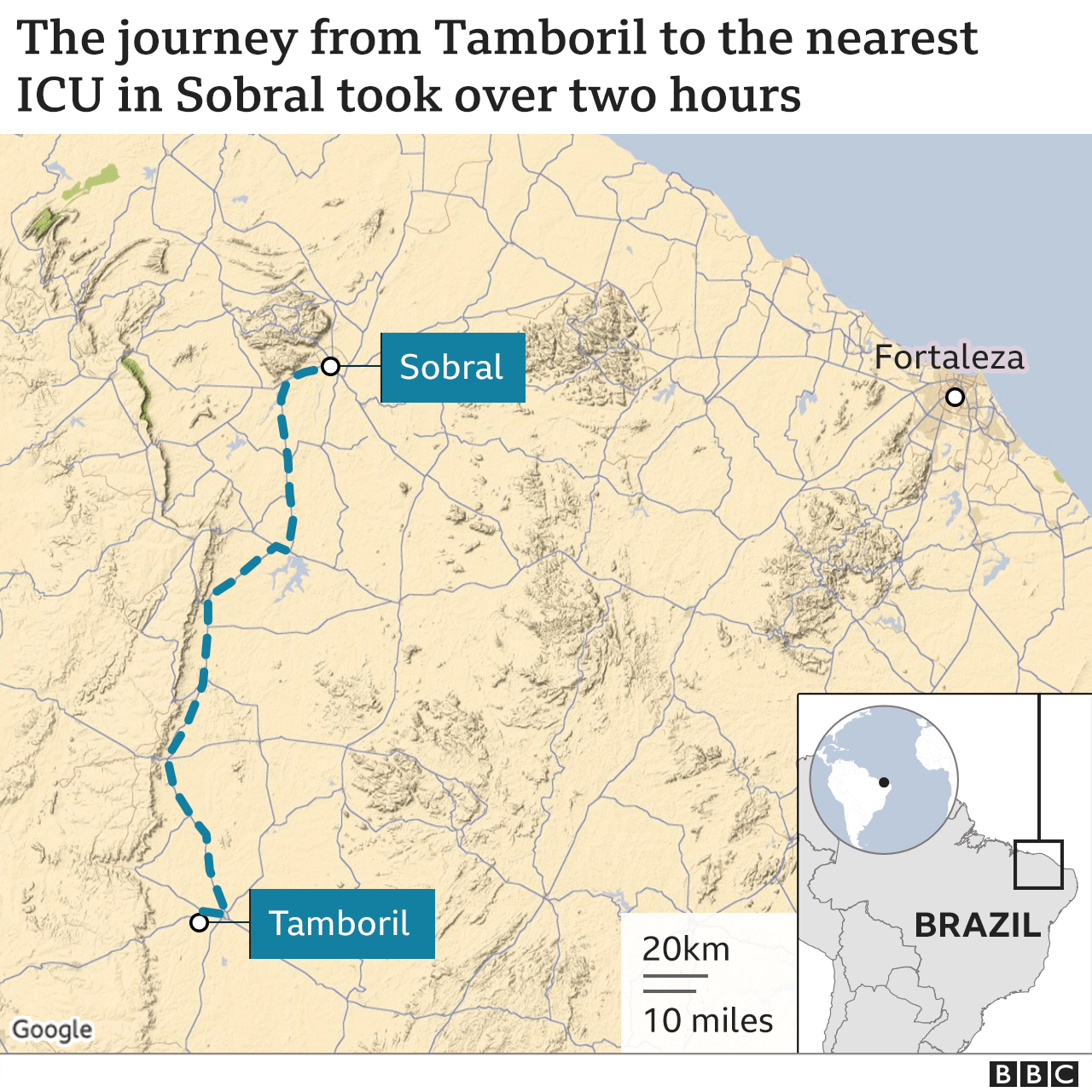
Lucas was transferred to a paediatric intensive care unit in Sobral, over two hours away, where he was diagnosed with a condition called multi-system inflammatory syndrome (MIS).
This is an extreme immune response to the virus, which can cause inflammation of vital organs.
Experts say the syndrome, which affects children up to six weeks after they are infected with coronavirus, is rare, but leading epidemiologist Dr Fatima Marinho from the University of São Paolo, says that, during the pandemic, she is seeing more cases of MIS than ever before. Although it doesn’t account for all deaths.
When Lucas was intubated, Jessika wasn’t allowed to stay in the same room. She rang her sister-in-law to try and distract herself.
“We could still hear the sound of the machine, the beep, until the machine stopped and there was that constant beep. And we know that happens when the person dies. After a few minutes, the machine started working again and I started to cry.”
The doctor told her Lucas had suffered a cardiac arrest but they had managed to revive him.
Dr Manuela Monte, the paediatric doctor who treated Lucas for over a month in the ICU in Sobral, said she was surprised that Lucas’s condition was so serious, because he did not have any risk factors.
Most children affected by Covid have comorbidities – existing conditions such as diabetes or cardiovascular disease – or are overweight, according to Lohanna Tavares, a paediatric infectologist at Albert Sabin Children’s Hospital in Fortaleza, the state capital.
But that wasn’t the case with Lucas.
During the 33 days Lucas was in the ICU, Jessika was only allowed to see him three times. Lucas needed immunoglobulin – a very expensive medication – to deflate his heart, but luckily an adult patient who had bought his own had donated one leftover ampoule to the hospital. Lucas was so ill that he went on to receive a second dose of immunoglobulin. He developed a rash on his body and was running a persistent fever. He needed support to breathe.
Then Lucas began to improve and the doctors decided to take out his oxygen tube. They video-called Jessika and Israel so that he wouldn’t feel alone as he regained consciousness.
“When he heard our voices he started to cry,” says Jessika.
It was the last time they were to see their boy react. During the next video call “he had a paralysed look”. The hospital requested a CT scan and discovered Lucas had had a stroke.
Still, the couple were told Lucas would make a good recovery with the right care and would soon be moved out of ICU and into a general ward.
When Jessika and Israel went to visit him, the doctor was just as hopeful as they were, she says.
“That night, I put my cell phone on silent. I dreamed Lucas came up to me and kissed my nose. And the dream was a great feeling of love, gratitude and I woke up very happy. Then I saw my cell phone and saw the 10 calls that the doctor had made.”
The doctor told Jessika that Lucas’s heart rate and oxygen levels had dropped suddenly, and he had died early that morning.
She feels sure that if Lucas had been given a Covid test when she had requested it back in early May he would have survived.
“It is important that doctors, even if they believe it is not Covid, do the test to eliminate the possibility,” she says.
“A baby does not say what he is feeling, so we depend on tests.”

Jessika believes that the delay in proper treatment made his condition more serious. “Lucas had several inflammations, 70% of the lung was compromised, the heart increased by 40%. It was a situation that could have been avoided.”
Dr Monte, who treated Lucas, agrees. She says that although MIS cannot be prevented, treatment is much more successful if the condition is diagnosed and treated early.
“The earlier he would have received specialised care, the better,” she says. “He arrived at the hospital already critically ill. I believe he could have had a different outcome if we could have treated him earlier.”
Jessika now wants to share Lucas’s story to help others who may miss critical symptoms.
“Every child I know was saved by some warning and the mother says: ‘I saw your posts, I took my son to the hospital and he is now at home.’ It’s as if it were a little bit of Lucas,” she says.
“I have been doing for these people what I wish they had done for me. If I had had information, I would have been even more cautious.”

There is a misconception that children are at zero risk for Covid, says Dr Fatima Marinho, who is also a senior adviser to the international health NGO Vital Strategies. Marinho’s research has found that a shockingly high number of children and babies have been affected by the virus.
Between February 2020 and 15 March 2021, Covid-19 killed at least 852 of Brazil’s children up to the age of nine, including 518 babies under one year old, according to figures from the Brazilian Ministry of Health. But Dr Marinho estimates that more than twice this number of children died of Covid. A serious problem of underreporting due to lack of Covid testing is bringing the numbers down, she says.
Dr Marinho calculated the excess of deaths by unspecified acute respiratory syndrome during the pandemic, and found that there were 10 times more deaths by unexplained respiratory syndrome than in previous years. By adding these numbers, she estimates that the virus in fact killed 2,060 children under nine years old, including 1,302 babies.https://emp.bbc.com/emp/SMPj/2.40.2/iframe.htmlmedia captionLooking after the babies and children in Brazil’s Covid ICU
Why is this happening?
Experts say the sheer number of Covid cases in the country – the second-highest number in the world – have increased the likelihood that Brazil’s babies and young children are affected.
“Of course, the more cases we have and, as a result, the more hospitalisations, the greater the number of deaths in all age groups, including children. But if the pandemic were controlled, this scenario could evidently be minimised,” says Renato Kfouri, president of the Scientific Department of Immunisations of the Brazilian Society of Pediatrics.
Such a high infection rate has overwhelmed Brazil’s entire health care system. Across the country, oxygen supplies are dwindling, there is a shortage of basic medicines and in many ICUs across the country there are simply no more beds.

Brazilian President Jair Bolsonaro continues to oppose lockdowns and the infection rate is being driven by a variant called P.1 which emerged in Manaus, in northern Brazil, last year, and is thought to be much more contagious. Twice the number of people died last month than in any other month of the pandemic, and the upward trend is continuing.
Another problem driving the high rates in children is a lack of testing.
Marinho says that for children often the Covid diagnosis comes too late, when they are already seriously ill. “We have a serious problem detecting cases. We don’t have enough tests for the general population, even fewer for children. Because there is a delay in the diagnosis, there is a delay in care for the child,” she says.
This is not just because there is little testing capacity, but also because it is easier to miss, or misdiagnose, the symptoms of children suffering from Covid-19, as the disease tends to present differently in younger people.
“A child has a lot more diarrhoea, a lot more abdominal pain, and chest pain, than the classic Covid picture. Because there is a delay in diagnosis, when the child arrives at the hospital they are in a serious condition and can end up complicating – and dying,” she says.
But it’s also about poverty and access to health care.
An observational study of 5,857 Covid-19 patients under the age of 20, carried out by Brazilian paediatricians led by Braian Sousa from the São Paolo school of medicine, identified both comorbidities and socioeconomic vulnerabilities as risk factors for the worst outcome of Covid-19 in children.
Marinho agrees this is an important factor. “Most vulnerable are black children, and those from very poor families, as they have the most difficulty accessing help. These are the children most at risk of death.” She says this is because crowded housing conditions make it impossible to socially distance when infected, and because poorer communities do not have access to a local ICU.
These children are also at risk of malnutrition, which is “terrible for the immune response”, Marinho says. When Covid payments stopped, millions were plunged back into poverty. “We went from 7 million to 21 million people below the poverty line in one year. So people are also going hungry. All of this is impacting mortality.”
Sousa says his study identifies certain risk groups among children that should be prioritised for vaccination. Currently, there are no vaccines available for children under 16 years of age.

Visits by relatives to children in ICU have been restricted since the beginning of the pandemic, for fear of infection.
Dr Cinara Carneiro, an ICU doctor at Albert Sabin Children’s Hospital, says this has been immensely challenging, not just because parents are a comfort to their children, but because they can also help in a clinical sense – they can tell when their child is in pain or in psychological distress and when they need soothing rather than medicating.
And she says the parents’ absence intensifies their own trauma when they hear their child’s condition has deteriorated and they haven’t been there to witness it.
“It hurts to see a child dying without seeing their parents,” says Dr Carneiro.
In an attempt to improve the communication between parents and their children, staff at Albert Sabin hospital clubbed together to buy phones and tablets to facilitate video calls.
Dr Carneiro says this has helped immensely. “We have made over 100 video calls between family members and patients. This contact has greatly reduced the stress.”
Scientists stress the risk of death in this age group is still “very low” – the current figures suggest only 0.58% of Brazil’s 345,287 Covid deaths to date have been of 0-9 year olds – but that is more than 2,000 children.
“The numbers are really scary,” says Dr Carneiro.

When to seek help
While coronavirus is infectious to children, it is rarely serious. If your child is unwell it is likely to be a non-coronavirus illness, rather than coronavirus itself.
The Royal College of Paediatrics and Child Health advises parents seek urgent help if their child is:
- Becoming pale, mottled and feeling abnormally cold to the touch
- Has pauses in their breathing (apnoeas), has an irregular breathing pattern or starts grunting
- Has severe difficulty in breathing, becoming agitated or unresponsive
- Is going blue round the lips
- Has a fit/seizure
- Becomes extremely distressed (crying inconsolably despite distraction), confused, very lethargic (difficult to wake) or unresponsive
- Develops a rash that does not disappear with pressure (the ‘Glass test’)
- Has testicular pain, especially in teenage boys
source : bbc.com



